The Medical Billing Process: What the 10 Steps Really Look Like in an Actual Practice
Everyone in healthcare has heard the term medical billing process, but if you ask ten different people to explain it, you will usually hear ten different versions. Some people think it begins with claim submission. Others believe it starts with coding. Some forget that the front desk is part of it too. That is where the confusion begins.
The medical billing process is not just a task handled by someone in the back office. It touches every department in a practice, from patient registration to collections. If one part breaks down, the entire revenue cycle feels the impact.
To understand how practices get paid properly, it helps to see what the medical billing process actually looks like from beginning to end.
What Are the 10 Steps in the Medical Billing Process and What Goes Wrong at Each One
There is always debate about how many stages belong in the medical billing process. Some people count eight. Others count twelve. In reality, most billing teams work through ten main steps.
| Step in the Process | What Actually Happens | Common Failure Point |
| 1. Patient registration | Demographic and insurance information is collected before the visit | Incorrect insurance details entered at the front desk |
| 2. Insurance eligibility check | Coverage, benefits, and limitations are verified before treatment | Eligibility is skipped and the claim gets denied later |
| 3. Encounter and documentation | The provider documents everything completed during the visit | Incomplete notes create coding issues later |
| 4. Medical coding | ICD-10-CM, CPT, and HCPCS codes are assigned to services | Missing modifiers or wrong codes trigger denials |
| 5. Charge entry | Coded services are entered into the billing software with fees | Duplicate charges or missing services reduce revenue |
| 6. Claim scrubbing | Claims are reviewed for errors before being sent to the payer | Scrubbing rules are too weak and mistakes pass through |
| 7. Claim submission | A clean electronic claim is sent to the payer | Claims are sent late or to the wrong payer |
| 8. Adjudication | The payer reviews, approves, denies, or reduces payment | Downcoded claims are accepted without appeal |
| 9. Payment posting | Payments are matched to the correct claim and posted | Payments are posted to the wrong accounts |
| 10. AR follow-up | Denied and unpaid claims are worked until resolved | Claims sit past 90 days and get written off |
Most billing issues do not begin in the billing department itself. They usually begin at step one when patient or insurance information is entered incorrectly. If that information is wrong from the start, the entire medical billing process is affected.
Medical Billing Process Flow Chart: How the Stages Connect
When people mention a medical billing process flow chart, they are usually referring to a visual outline of the ten steps. However, in real life, the process is not a straight line.
The medical billing process includes multiple decision points. Claims can be denied and sent back for correction. Payments can be reduced and appealed. Certain issues loop backward before moving forward again. It works more like a connected system than a simple checklist.
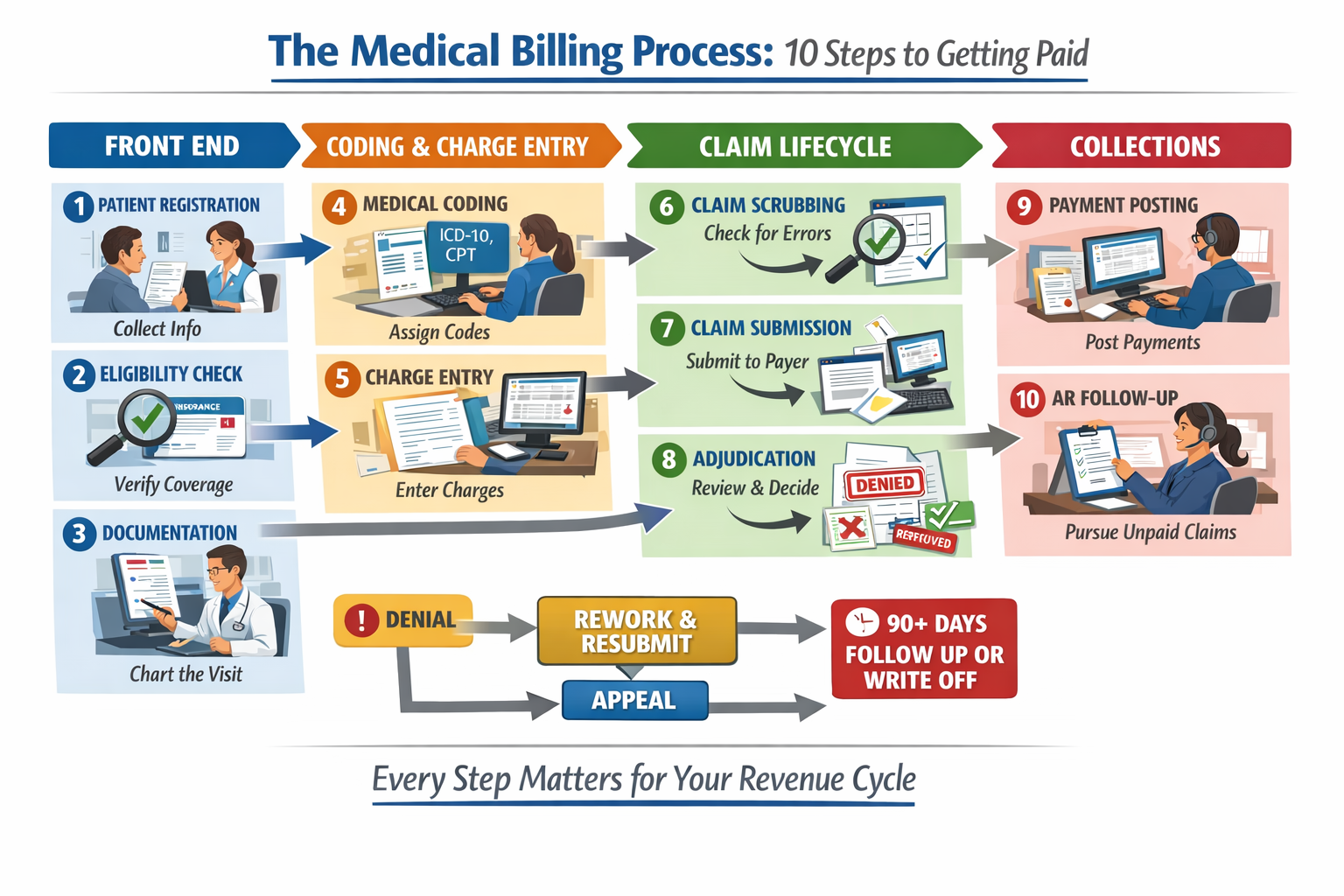
The easiest way to understand it is by dividing the medical billing process into four larger phases.
| Phase | Steps Covered | Who Owns It | What Can Go Wrong |
| Front end | Steps 1 to 3 | Front desk and clinical staff | Incorrect information leads to bad claims |
| Coding and charge entry | Steps 4 to 5 | Medical coders and billers | Coding mistakes create denials and compliance risks |
| Claim lifecycle | Steps 6 to 8 | Billing staff and payers | Claims miss filing deadlines or go to the wrong payer |
| Collections | Steps 9 to 10 | AR specialists | Aging claims sit too long without follow-up |
The front end controls everything that happens later. If patient registration is incomplete or eligibility is not verified, that error continues through coding, scrubbing, submission, and collections.
By the time the claim is denied, the practice may need hours to trace the issue back to a small registration mistake made weeks earlier. Many practices with high denial rates actually have a front-end problem rather than a billing problem.
A medical billing process flow chart only works if every department understands how their part affects the next stage. The front desk does not need to know coding rules in detail, but they do need to understand why accurate insurance information matters.
The Parts of the Medical Billing Process That Usually Break
Some parts of the medical billing process fail more often than others and cost practices a large amount of money.
One of the biggest issues happens at step two, insurance eligibility verification. Many practices either skip this step or wait until the patient arrives. By then, there is little time to fix coverage issues. The patient is seen, the claim is sent, and later it is denied because the insurance coverage had already expired.
Step eight is another common weak point. During adjudication, the payer may approve the claim but reduce the payment amount. For example, a claim submitted as a level four visit may come back paid as a level three visit.
If no one compares the explanation of benefits to the original claim, the reduced payment is accepted automatically. Over time, those small losses add up quickly.
Step ten, AR follow-up, is often the most ignored part of the medical billing process in smaller practices. Claims remain in the 90-day bucket without action. Nobody follows up. The timely filing deadline passes. Once that happens, the revenue is usually lost for good.
If most practices could improve only one part of the medical billing process, it would probably be AR follow-up. A strong process for working unpaid claims before they age out can recover a significant amount of lost revenue.
Why Getting the Medical Billing Process Right Matters
The medical billing process is not only about collecting payments. It also shows how healthy a practice is financially.
A practice with low denial rates, fewer AR days, and a clean claim rate above 95 percent usually has stable cash flow. That allows the practice to hire staff, invest in equipment, and continue growing.
A practice with poor billing performance may have a full patient schedule but still struggle financially because revenue is leaking out at multiple stages.
That is what many people overlook. Even busy practices can face cash flow problems if the medical billing process is not working properly.
So What Should You Do Next
If you reviewed these ten steps and noticed a few problems that sound familiar, it may be time to look more closely at your current system.
The medical billing process can usually be improved once the weak points are identified. Reviewing denial rates, AR aging, clean claim rates, and front-end workflows can quickly show where revenue is being lost.
Whether you manage the medical billing process in-house or work with an outside billing company, the same rule applies. Every step matters. The order matters. And the information passed from one stage to the next must stay accurate or the entire system will underperform.